Red Snappers
Making a challenging diagnosis
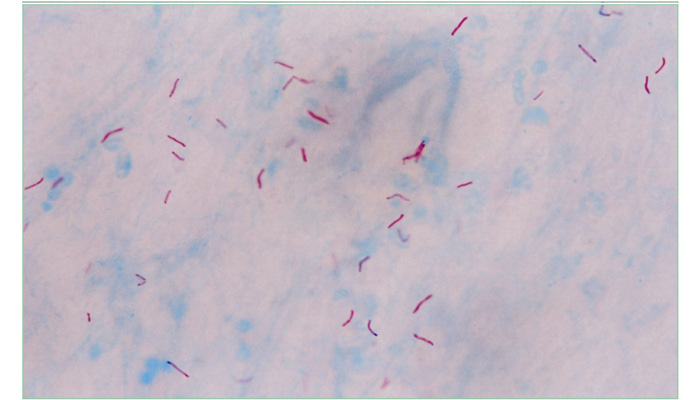
Photomicrograph of red-staining Mycobacterium tuberculosis organisms (“red snappers”) against a methylene blue background. Image in the public domain, content provider: CDC/Dr. Goerge P. Kubica. https://phil.cdc.gov/PHIL_Images/20040615/d094324845a24eb3a7bfe0d1f8e4a637/5789_lores.jpg
One of the exhilarations that comes with being a doctor is making a challenging diagnosis, especially when it was missed by other doctors and leads to life-saving results. The experience is not so much a demonstration that you’re smarter than your colleagues but more that by careful reasoning you make a huge difference in a patient’s outcome. The first time I experienced this emotion was nearly 50 years ago.
It was my senior year in medical school. I had chosen to do a one-month elective in pulmonary medicine at our county hospital, where most patients were poor and medical students got lots of hands-on experience. My resident and I had finished morning rounds and were eating lunch when the emergency room paged. “They’re sending us a 56-year-old man with a lung abscess. The emergency room doctor said the x-ray was classic,” she reported. We quickly finished lunch. While she assessed the patient, I hurried to the medical library to read about lung abscess. I wanted to be prepared. Then it was my turn. I took a history, performed a physical exam, and reviewed the patient’s chest x-ray.
“So, what do you think?” my resident asked with just the hint of a wry smile.
“Well, his x-ray shows a cavitary infiltrate in the right lung. It looks like the x-rays I saw when reading about lung abscess,” I replied, wanting her to know I had just researched the topic of lung abscess.
“That is true.” My resident paused and then added, “But don’t start with the x-ray. It can lead you to an early conclusion and close your mind to other diagnostic possibilities. Go back to your own history and physical exam. What symptoms does the patient have?”
Now less confident, I replied, “Well, he’s had cough and night sweats for a few weeks. And he’s lost weight.” I had just read that these symptoms were often reported by patients with a lung abscess.
“Good. And is there anything special about the sputum in patients with lung abscess?”
“Well, it’s supposed to be purulent, and foul smelling,” I replied.
“And what are exam features in persons with lung abscess?” she asked.
“Patients with lung abscess frequently have poor dentition and a fetid breath. The lung infection often originates from a dental source.” I had now nearly exhausted what I’d learned about lung abscess during my few minutes of library research.
“Now, take what you know about lung abscess and apply it to this patient,” she said. “Ask yourself, do my history and physical exam findings fit with the diagnosis of lung abscess?”
I thought back about what I had found during my interview and physical exam. “He said his sputum didn’t smell bad but was bloody. When I examined him, I didn’t notice bad breath. And he didn’t have poor dentition. In fact, he was edentulous. So his history and physical exam don’t fit really well.” My resident remained silent while I worked through the diagnostic reasoning. “If a lung abscess originates from a dental infection, I guess it’s unlikely for an edentulous person to get a lung abscess. So the history and exam are not as typical as his x-ray.”
“Correct,” my resident said. “And what else, other than a lung abscess, can cause a cavitary infiltrate on x-ray?”
I searched my memory and then smiled. “TB” I shouted.
“Bingo,” said my resident. She returned my smile. “I don’t think our patient has a lung abscess. I think he has tuberculosis which can look like a lung abscess on x-ray. Tuberculosis causes cavitary lung disease and can cause bloody sputum.” She was excited, and so was I. It would be the first time I’d seen a patient with suspected tuberculosis.
My resident added, “I think the ER doc looked at the x-ray first and already had the diagnosis of lung abscess in mind before he evaluated the patient. So his thinking stopped there. He didn’t consider that this might be something else. I’m not criticizing him. It’s an easy thing to do. We often have information before we see patients, like an x-ray or another doctor’s diagnosis. That shapes our thinking. But I believe it’s important to start with your own history and exam, and then ask yourself if that fits with the imaging or the other doc’s diagnosis. That’ll help keep you out of trouble.”
Excited to test her hypothesis, I returned to the patient’s bedside, gathered a sputum specimen and hurried to the small lab housed in the resident work room. I placed some of his sputum on a microscope slide, allowed it to dry and then proceeded to do a Kinyoun stain. This technique, designed to identify tuberculosis organisms in clinical specimens, was developed in 1915 by Dr. Joseph Kinyoun, who founded the United States Hygienic Laboratory, predecessor of the National Institutes of Health. The bacteria that cause tuberculosis (Mycobacterium tuberculosis) have very thick cell walls containing a waxy lipid called mycolic acid. This allows them to be stained with certain dyes that resist decolorization by acid-alcohol. It is why they are called acid-fast.
I carefully flooded the slide with red carbolfuchsin, rinsed it, flooded it with acid alcohol, rinsed it again, and then doused it with methylene blue. After allowing it to dry, I applied a cover slip, added a drop of oil and then eagerly examined it under the lab’s oil-immersion microscope. Slowly focusing the high magnification lens up and down, the stained sputum came into view, and then suddenly, there they were—so-called red snappers, red-staining Mycobacterium tuberculosis organisms, the culprit of my patient’s illness—proving our diagnosis and allowing us to prescribe the correct treatment. My resident heard my shouts of excitement, ran to peer into the microscope, and echoed my exclamations of joy. We informed the patient and prescribed appropriate antituberculosis antibiotics. Within a few days he was feeling better, his sputum cleared and his appetite improved. After discharge he completed several months of antibiotics and was cured.
We don’t teach the Kinyoun staining technique to medical students anymore. There are no microscopes in my hospital’s resident work rooms. Sputum exams are done by certified technicians in the accredited hospital lab using more reliable methods, bills are sent to insurance companies, and official results are posted to the electronic health record, not recorded solely in the medical student note, written with an excited hand.
At the time, I didn’t appreciate how effective a teacher my resident had been. She could have just told me that she thought the patient had tuberculosis. But instead, she walked me through the deductive reasoning and allowed me to derive the correct answer for myself. And before it had a name, she taught me about something we would later call anchoring bias, a decision-making process that can lead to errors because it relies too heavily on an initial piece of information and alternative diagnoses are not considered. Though I no longer need to do Kinyoun stains or peer into microscopes, this instructive experience remains a vivid memory and served me and my patients for years to come.
Author’s note. An edited version was accepted for publication in the Journal of Graduate Medical Education. Sincere apologies to those who find this is too technical and not very interesting. I hope to do better in future posts for my non-clinical readers.


Not too technical, and very interesting!
How fun! Thanks for the walk down memory lane. I remember as a jr student diagnosing acute MI in a lady who couldn’t finish her pies before Thanksgiving . No other physical clues
It was my first big thrill and came from careful H&P